Radiation Oncology
NC State radiation oncologists can deliver radiation treatments with extreme precision, which result in decreased normal tissue side effects and the ability to increase the radiation dose to the tumor, hopefully improving tumor control.
Overview
A diagnosis of cancer in pets is increasingly common as our companion animals live longer due to a lifetime of excellent care. Although cancer can occur in pets of any age, there is an increasing risk of most cancers with age. Pet owners should be vigilant about looking for clinical signs that could be related to cancer, such as non-healing wounds, lumps or bumps on the skin or in the mouth, and lameness. It is the task of veterinarians to examine and investigate the underlying cause of such abnormalities. A diagnosis of cancer may come from a blood test, x-rays, or needle aspirates of lesions. Once a pet is diagnosed or suspected of having cancer, a veterinary oncologist is the health professional best trained to further stage and recommend treatments for your pet’s disease.
Typically, cancers may be treated with combinations of surgery, chemotherapy, radiation therapy, and sometimes immunotherapy. In the past, radiation therapy was commonly used to treat cancers that were non-resectable by surgeons or for tumors that were incompletely removed at surgery. Although radiation is still used in this way today, the advent of many new technologies that we now have available at NC State now allows us to consider radiation therapy for cancers that were previously thought to be untreatable, such as large liver tumors or metastatic brain tumors.
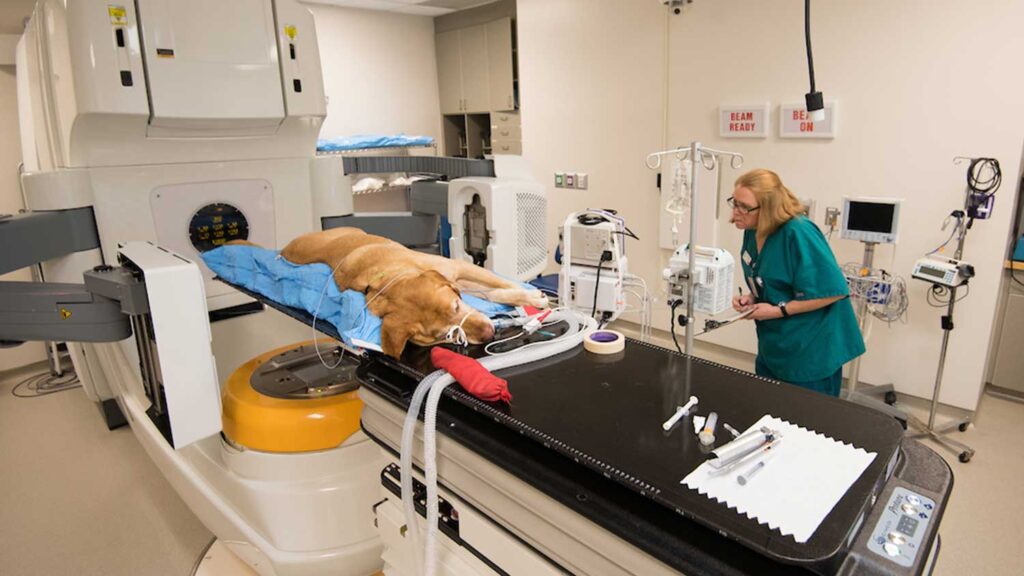
We are fortunate to have cutting-edge technology available in the form of a Varian Novalis TX linear accelerator with a Protura six-degrees-of-freedom treatment couch. This allows us to deliver radiation treatments with extreme precision, which results in decreased normal tissue side effects and the ability to increase the radiation dose to the tumor, hopefully improving tumor control. We can deliver radiation via photons or electrons, using both traditional (electron beam and clinical photon radiation plans) and cutting-edge radiation treatment plans (stereotactic radiation therapy (SRT) and intensity-modulated radiation therapy (IMRT)).
What makes NC State radiation oncology special?
- We are experts. We care for more than 200 cases per year.
- Radiation Oncologist Dr. Tracy Gieger is certified in three medical specialties — Internal Medicine, Medical Oncology and Radiation Oncology.
- Radiation Oncologist Dr. Mike Nolan, in addition to being board-certified in his specialty, has a Ph.D. in radiation and cancer biology and runs a vigorous research program.
- NC State’s collaboration with other institutions — such as the Consortium for Canine Comparative Oncology with Duke University — brings top minds together to explore new cancer therapies offering better efficacy and less toxicity for both animals and humans.
- Despite the rapid change of the increasingly effective technology, we work hard to stay at the cutting edge of what is available in order to provide the most effective treatment, and the highly experienced team employs these tools with great skill and precision.
- The Radiation Oncology team understands that we don’t simply treat animal cancers, we treat whole families. We approach client care with this holistic view.
Contact Us
- Hours: Monday through Friday, 7:30 a.m to 4:30 p.m
- Phone: 919-513-6690
- Email: ncstateoncology@ncsu.edu
Common Cancers and How We Teat Them
- Bladder & Prostate Cancer
- Bone Cancer
- Brain Tumors
- Cardiac Hemangiosarcoma in Dogs
- Chemodectomas (Heart-Base Tumors) in Dogs
- Feline Acromegaly, Pituitary tumors in Cats
- MLO in Dogs
- Lung Cancer in Dogs and Cats
- Nasal Cancer
What to Expect
The Radiation Oncology service is a referral-only service. Once the primary (referring) veterinarian calls and sets up the referral, the owner may call and arrange an appointment. If your veterinarian has confirmed the diagnosis of cancer in your pet, have he or she call our hospital and discuss your pet’s case with the Radiation Oncologist. In some tumor locations, especially for suspected brain tumors, a biopsy diagnosis is not required for consideration of radiation therapy.
Appointments and Referrals
Appointment Guidelines
At the time of your appointment, the radiation oncologists will discuss the additional tests that are recommended or required prior to radiation treatment, the options and expected outcomes for radiation therapy, and the costs and potential side effects associated with treatment.
Many patients undergo radiation therapy (RT) on an outpatient basis. This means that if they are medically stable, there is usually no need to keep them overnight. Depending on the type of treatment being given, your pet may need RT to be given as often as five days per week (Monday through Friday) for three to five consecutive weeks.
Effective as of February 15, 2023, the Radiation Oncology service requires a 24 – 48 hours notice of cancellation of all appointments, in order to not incur a missed appointment fee. You may notify us by email: ncstateoncology@ncsu.edu or a phone call to the Front Desk at 919-513-6690
Thank you for your understanding.
Appointment Hours
Housing and Transportation Options During Radiation Therapy.docx (N0015128.DOCX;1)
Generally, patients are dropped off each morning between 7:30 and 8:00 a.m. Then, after the day’s treatment is done, and the patient has fully recovered from anesthesia, we call with an update, and to schedule a time for them to be picked up. This can be as early as 9:30 a.m., or as late as about 6:00 p.m., but generally is around 2:00 – 4:00 p.m.
Estimated Costs
- Initial Consultation appointment with the radiation oncology service: $287
- Palliative radiation therapy (typically 1-6 treatments): $875-4000
- Definitive course of radiation therapy (if no CT scan required; typically 15-19 daily treatments): $4500-6000
- Course of radiation therapy delivered with intensity-modulated radiation therapy (IMRT) (typically 18-20 daily treatments): $6700-8500
- Course of stereotactic radiation therapy (SRT) (typically 1-3 treatments delivered over 1-5 weekdays): $6000-7000
Frequently Asked Questions
When am I going to see a doctor?
Please note that our Interns and Residents (aka House Officers), are fully licensed doctors with the same education and credentials as a general practitioner. There will ALWAYS be a doctor in charge of and supervising all aspects of patient care at the VH. In many cases multiple specialists may consult on a patient should their expertise be required. Typically, a fourth-year student will first collect a detailed history and present this information to the doctor in charge. You will then have an opportunity to discuss things in detail with the doctor and together you and he/she will formulate a diagnostic and treatment plan.
Can I board my pet in your hospital while they’re undergoing treatment?
Please know that if it’s a service you would like to take advantage of, we are able to board most patients in the hospital from Monday through Friday. This adds approximately $50 per night, for most pets. We can also provide care over the weekend for patients that have a medical need. However, we cannot offer general boarding services over the weekend; this is only available from 7:30 a.m. Monday morning through 6:00 p.m. Friday evening.
What happens if I can’t get to the hospital during the designated Friday pick-up time, and Monday drop-off time?
There are local small businesses which can provide boarding over the weekend. These businesses can also provide transportation to and from our hospital for cancer care. These businesses are independently licensed, bonded and insured. You will need to contact these businesses to make arrangements, and to discuss logistics, including cost.
With your permission, we can discharge your pet to an employee or agent working for one of these businesses. We can even communicate with them, to ensure they understand special medicalneeds that may arise as your pet undergoes treatment (such as new medications that are being prescribed, changes in drug doses, need for special wound care, etc.).
The following are businesses identified as offering boarding services and transportation. NC State Veterinary Hospital does not endorse or recommend any commercial products, processes, or services, and reference herein to any specific business does not constitute or imply its endorsement, recommendation, or favoring by NC State.
Current businesses that may be able to offer these services to you include:
Penny Pinching Pooches
- Contact Name: Sherrill Jacobson
- Phone: (919)601-0233
- Email: pppooches@yahoo.com
- Web Address: Penny Pinching Pooches
What does it mean to be a ‘teaching hospital’?
In addition to having access to cutting edge diagnostic tools and therapeutic alternatives, the most unique aspect of our facility is that every patient is a learning opportunity for our students. Much of this teaching is done ‘behind the scenes’ as we discuss your pets’ diagnostics and care. What this means to you, the client, is that the process may take somewhat longer than it would at a private veterinarian practice. However, this also means that we have the ability to consult with multiple doctors and a variety of specialists in complex cases.
My doctor introduced him/herself as an Intern or a Resident – what does that mean?
It is important to understand that every intern or resident at the VH is a fully licensed doctor with the same education and credentials as a general practitioner. Interns and residents have chosen to pursue additional, in-depth postgraduate clinical training and were selected by us in a highly competitive international application process. We think you are in great hands!
Is there food and water available for my pet while I wait?
Feel free to ask the front desk for a bowl if you would like to offer water to your pet. However, we do ask that you refrain from feeding your pet. Many procedures require sedation or medication with drugs that could upset your companion’s stomach if there is food present. If your pet must eat for medical reasons (eg. diabetes), please ask the front desk to inform the doctor in charge and make sure they are aware of this first.
I am finished with my visit, why do I have to wait?
One of our goals for our clients is that everyone leaves with detailed discharge instructions. We write our discharge instructions in as detailed manner as possible to help summarize the information covered during the visit and give you specific instructions as to medications, diet, activity restriction, and any other pertinent aspect of care. It may take us some additional time to write these for you; however, this can significantly ease the transition home and back to your regular veterinarian.
You are a State facility, so why are your fees so high?
The VH is a not-for-profit health care center and receives less than 2% of operating costs from the the State of North Carolina. The majority of our operating costs are paid by client fees and donations. In fact, many of the state-of-the-art diagnostic and treatment options we offer are only possible because of generous gifts from our clients. Our fees are set to cover the balance of our operating costs, and we are always looking for ways to provide better service at lower cost. Total costs are comparable to those of veterinarian specialists in private practice.


